Group leader Dr. Marieke Essers (PhD)
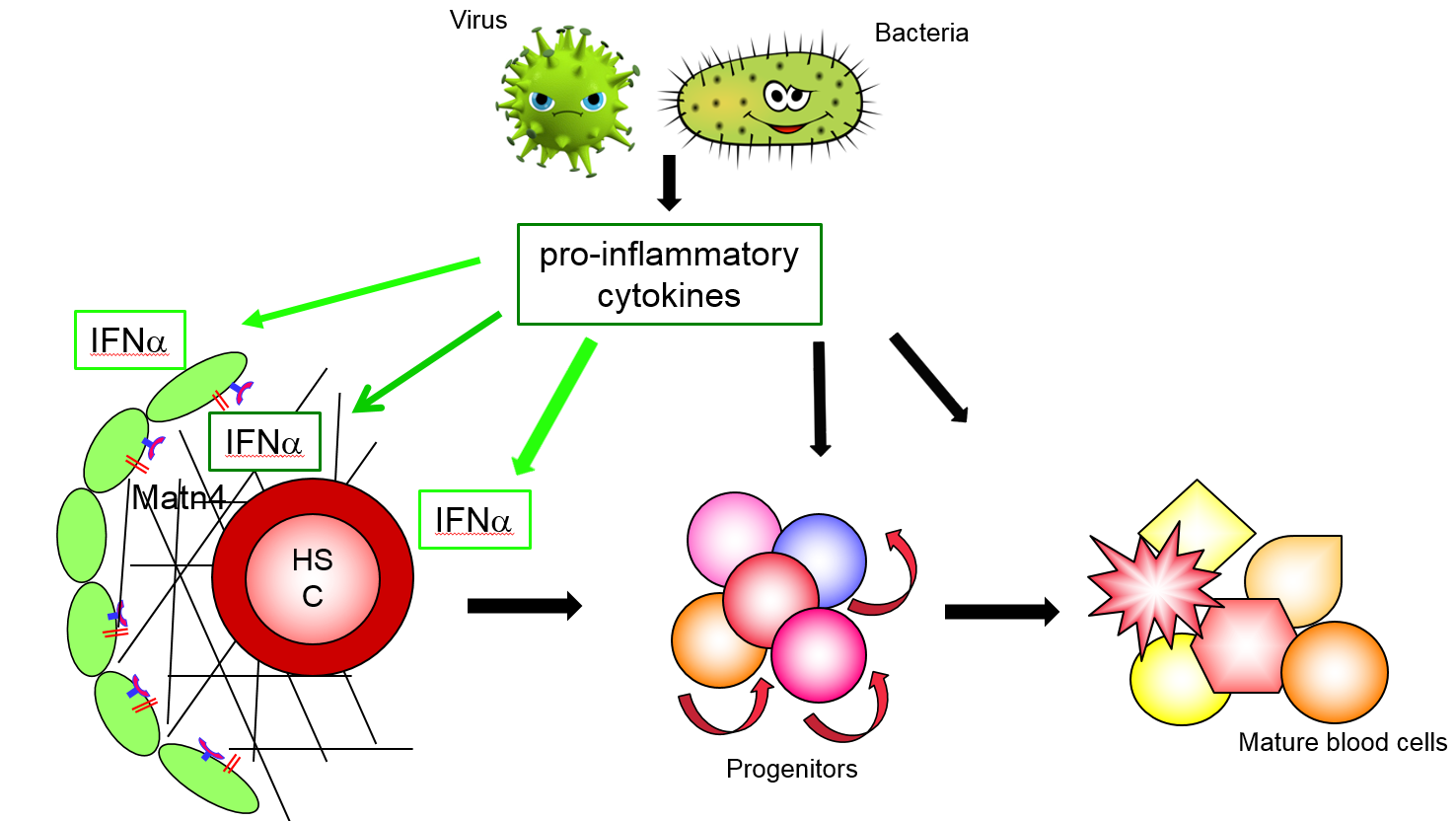
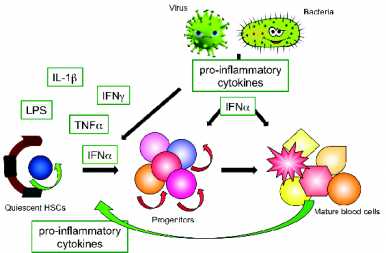
Pro-inflammatory cytokines link infection and inflammation to quiescent Hematopoietic Stem Cells (HSCs), leading to their activation.
Infection is a common, natural form of stress, with which the body is regularly challenged. During infection or inflammation, cells of the immune system are responsible for fighting the invading pathogens, leading to high consumption of blood and immune cells. Restoration of the balance of the hematopoietic system following successful elimination of the infection is a crucial part of the recovery of the body. In addition, both clinical and experimental data indicate that depending on the scale and duration, infection and inflammation can induce hematopoietic dysfunction compromising immune defense mechanisms and possibly contributing to the development of hematologic malignancies.
Restoring the balance of the hematopoietic system depends on the replacement of lost immune cells by hematopoietic stem cells (HSCs). Over the years, the biology of HSCs and their progeny has been studied in great detail during homeostasis. However little is known about how stress scenarios, such as infection-induced inflammatory responses, impact on HSC self-renewal and differentiation, controlling emergency hematopoiesis.
The focus of our research is to understand the link of inflammation and the hematopoietic stem cell (HSC) compartment via the effect of the pro-inflammatory cytokines on quiescent HSCs and their niche. The group focuses on three main themes:
- the inflammatory response of HSCs in vivo
- the response and role of the bone marrow niche under inflammatory stress
- activation of leukemic stem cells by pro-inflammatory cytokines
The data we’ll generate in these projects will further our understanding on the mechanisms by which HSCs are reassuring the successful restoration of the blood system and how are HSCs protected from pathogenic insults. This will help us to better understand the response observed in patients with an intact, but also a compromised immune system, in which infection often lead to a severe disease. In addition, it might also open up possibilities to target quiescent leukemic stem cells (LSCs) for activation, making them susceptible to chemotherapy.
Selected Recent Publications
- Hirche C., Frenz T., Haas S., Döring M., Borst K. Tegtmeyer P., Brizic I., Jordan S., Keyser K., Chhatbar C., Pronk E., Lin S., Messerle M., Jonjic S., Falk C.S., Trumpp A., Essers M.A.G., Kalinke U. (2017). Systemic Virus Infections differentially modulate Cell Cycle State and Functionality of Long-Term Hematopoietic Stem Cells In Vivo. Cell Reports 19: pp2345-56
- Velten L.*, Haas S.F.*, Raffel S.*, Blaszkiewicz S., Islam S., Hennig B.P., Hirche C., Lutz C., Buss E.C., Nowak D., Boch T., Hofmann W.-K. Ho A.D., Huber W., Trumpp A.#, Essers M.A.G.#, Steinmetz L.M.#. (2017). Human haematopoietic stem cell lineage commitment is a continuous process. Cell Biol. 19: pp271-281
* shared first author, # shared last and corresponding author
- Prendergast A.M., Kuck A., van Essen M., Haas S., Blaszkiewicz S., Essers M.A. (2017). IFNa mediated remodeling of endothelial cells in the bone marrow niche. Haematologica, 102: pp445-453
- Uckelmann H., Blaszkiewicz S., Nicolae C., Haas S., Schnell A., Wurzer S., Wagener R., Aszodi A., Essers M.A. (2016). Extracellular matrix protein Matrilin-4 regulates stress-induced HSC proliferation via CXCR4. J Exp. Med. 213: pp1961-1971
- Haas S., Hansson J., Klimmeck D., Loeffler D., Velten L., Uckelmann H., Wurzer S., Prendergast Á.M., Schnell A., Hexel K., Santarella-Mellwig R., Blaszkiewicz S., Kuck A., Geiger H., Milsom M.D., Steinmetz L.M., Schroeder T., Trumpp A., Krijgsveld J., Essers M.A. (2015). Inflammation-induced emergency megakaryopoiesis driven by hematopoietic stem cell-like megakaryocyte progenitors. Cell Stem Cell 17: pp422-34
- Essers M.A.G., Offner, S., Blanco-Bose W.E., Waibler Z., Kalinke U., Duchosal M.A., and Trumpp A. (2009). IFNa activates dormant HSCs in vivo. Nature 458: pp904-908